Article Topics
 The use of medical cannabis for the effective treatment of nausea has been well documented for quite some time. However a novel set of characteristic symptoms that lead to an apparent increase in nausea has recently (2004) been coined. This paradoxical condition is known as Cannabinoid Hyperemesis Syndrome (CHS).
The use of medical cannabis for the effective treatment of nausea has been well documented for quite some time. However a novel set of characteristic symptoms that lead to an apparent increase in nausea has recently (2004) been coined. This paradoxical condition is known as Cannabinoid Hyperemesis Syndrome (CHS).
Cannabinoid Hyperemesis is exactly what you might think it is: exaggerated emesis (vomiting) with cannabis use. The recognition of this condition arose from clinicians recognizing a common cluster of symptoms in a relatively small population of chronic, heavy, and regular cannabis users.
The typical patient profile tends to be a regular user (i.e. daily consumption over an extended period of time such as one year or more). The nausea and vomiting was predominantly in the morning, lasted hours to days, and might recur cyclically over weeks to months. Many had 7 or more episodes a year. Yuck!
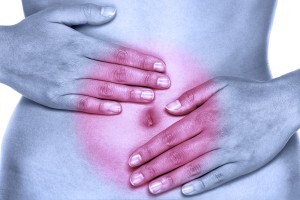
The typical patient profile presenting to their provider might offer the following story: “I had to come into the ER because I ran out of hot water at home, and I was afraid my nausea and vomiting would not stop. A long hot shower or bath was the only thing that helped.” Hmmm…?? A hot shower was all that it took to relieve their symptoms? Patients may also have experienced some abdominal pain, and typically had nothing else in their history or on their exam that indicated another specific cause to explain their symptoms. Patients seemed to find out on their own, that long hot showers or baths relieved their symptoms.
had to come into the ER because I ran out of hot water at home, and I was afraid my nausea and vomiting would not stop. A long hot shower or bath was the only thing that helped.” Hmmm…?? A hot shower was all that it took to relieve their symptoms? Patients may also have experienced some abdominal pain, and typically had nothing else in their history or on their exam that indicated another specific cause to explain their symptoms. Patients seemed to find out on their own, that long hot showers or baths relieved their symptoms.
When a loved one has nausea and vomiting, often the helpful thing we would want to provide would be a cold compress to the forehead, right? So does a hot shower seem counterintuitive?
Why would a hot bath or shower make these patients feel better?
Brain receptors that likely relieve nausea are probably the same culprits in producing a “paradoxical effect” (meaning that it has the opposite effect as the one intended) in this group of patients. A paradoxical effect with respect to a medically prescribed chemical is that it has the opposite effect as the one intended. For example, maybe you are aware that a common over the counter medication, such as Benadryl, can sometimes be taken at night for its sedative effects to help one sleep. Well, paradoxically, in some patients, it actually keeps them awake.
 If someone were to have an adverse effect to a substance, often we would imagine or anticipate that it would show up early on when using it. However, just like some food allergies, it may take repeated exposures before the body has an acquired hypersensitive response. With CHS in particular, it is important to consider it even after long term regular use without these symptoms, which makes its recognition tricky.
If someone were to have an adverse effect to a substance, often we would imagine or anticipate that it would show up early on when using it. However, just like some food allergies, it may take repeated exposures before the body has an acquired hypersensitive response. With CHS in particular, it is important to consider it even after long term regular use without these symptoms, which makes its recognition tricky.
What’s more, the typical medications used to treat nausea and vomiting don’t seem to help these patients. Are you confused about this condition yet?
What to do?
Initially, supportive therapy is provided, meaning intravenous fluids are given to correct dehydration caused by the vomiting. Other creative treatments are documented in the literature. So, it is important for patients to know the signs of dehydration as an indication of the need to seek medical treatment. These may include: dry mouth, thirst, reduction in urination frequency and the appearance of concentrated or dark urine, dizziness, lack of energy, confusion, and a faster than normal heart rate.
So…..are you wondering what the long term treatment is? It seems to be cessation of the use of cannabis. Just like other medically prescribed pharmaceuticals, sometimes patients just develop side effects that are intolerable.
the use of cannabis. Just like other medically prescribed pharmaceuticals, sometimes patients just develop side effects that are intolerable.
Why should this article demand our attention? Cannabis is a widely used drug of choice throughout the world. More and more, its use as a medically prescribed agent is becoming more accessible and acceptable. In 2008, the World Health Organization estimated the lifetime prevalence of the use of cannabis in the US was about 44%. Given the relatively new recognition of this condition, there remains a lack of information and awareness about CHS – among medical professionals as well as patients. It is likely that if chronic, regular cannabis use increases, the number of people experiencing this may increase too.
There is no current clinical test or other method to clearly diagnose this condition. History is key!
Sometimes patients are reluctant to or don’t think it is important to tell their health care providers about their use of cannabis or other herbal remedies or supplements. It is imperative that health care providers help their patients understand why supplying that specific information is important. For example, anything the patient takes in on their own, whether that be cannabis or any other type of substances, may interact with medications that are prescribed.
Educate.
 Both patients that use cannabis, and clinicians that treat patients that use cannabis must be aware of this condition. The down side to not recognizing CHS is ongoing symptoms, emergency room visits, and potentially unnecessary diagnostic tests, and even exploratory surgeries.
Both patients that use cannabis, and clinicians that treat patients that use cannabis must be aware of this condition. The down side to not recognizing CHS is ongoing symptoms, emergency room visits, and potentially unnecessary diagnostic tests, and even exploratory surgeries.
The exact frequency of this side effect of chronic cannabis use is difficult to know. Perhaps with more recognition of the condition and reporting of it, this information will become better well known.
It is our wish at UPG that our blogging is a reliable, timely, consistent, and informative way for you to stay abreast of current issues related to cannabis use. We would love to hear your thoughts. Have you had any experience (or think you may have) with CHS? Leave us your comments below, or on our Facebook, Twitter or other social media pages!



































This is interesting! I do occasionally feel very sick and sometimes throw up, but I have never correlated a hot shower with relief. I have blamed it on blood sugar, not drinking enough water. I even wondered if it was a “withdrawal symptom” because of not using enough cannabis oil. I have been taking the oil in varying amounts for over 2 years. My lung cancer is “stable” with only some tiny spots in my lungs that are too small to biopsy and are assumed to be cancer. They have been there the whole time (7+ years) but are smaller now. There is no cancer outside of my lungs as far as anyone can determine.
Could this condition have levels or stages of severity? IDK…I’m not planning on ever stopping the CO. I take it by suppository so I can function. Only eat a little on the weekends for fun and relaxation.
It does. The latest stage can cause gastroparesis (a paralyzed stomach) it can also leave you sweating for no reason. In my case the vomiting stopped a while ago. If you have cancer i wouldn’t quit weed if i were you
My husband started smoking pot when he was 16 in 1974 he died in 1992. We never new what his diagnosis was. After many hospitals, exploratory surgery, many different kinds of doctors,all kinds of medication,(one internal medicine doctor said”I gave him enough thorazine to knock out an elephant and he is still puking his guts out.”),many terrible months and also great ones,two great sons,divorce, and I won’t forget the key word SHOWERS,I finally learned what he died from in 2015. I can not tell you how much this grieves me to think this is what took my husband and father of my son’s away.He was a hard working good man that smoked pot. At least now I know what it was. One day I Googled,Excessive weight loss,vomiting and Hot showers and it came up HCS. It would be nice to talk to someone about this because this was a nightmare for our family and friends.
Hello Tammi, my heart truly does go out to you and I am sorry for your loss. Hopefully you will see this comment, though it has been a few months since you posted. I am 33 years old and I have been dealing with cyclical vomiting and abdominal pain since I as about 18 years old. I was really in the dark about what was going on and would frequently call the ambulance for dry heaving and throwing up bile. At first it seemed quite random, however years on down the road I started to notice that it was predominantly in the morning when I would wake up. Eventually I had an upper endoscopy done that would reveal a hiatus hernia and also signs of Barrett’s Esophagus condition. Needless to say I was a little scared after reading that BE was a precancerous condition that needed to be monitored to make sure it did not become cancer. However I felt like I was onto something, I felt I had an answer, at least they had found something that I could possibly improve and start to feel better. The next endoscopy I had done revealed significant healing, in fact the physician said there weren’t even any signs of BE anymore. I was happy about that, but still getting sick from time to time.
I am not sure when I first learned about the cannibinoid hyperemesis condition. To be honest it seemed very laughable to me, especially when I knew that pot was my go to when I felt sick, and it never failed to make me feel better. But the showers… there’s just no denying. I am also not sure when I discovered hot water relief from symptoms, it just sort of happened. Baths seemed to help more because I could just lay there and not worry about the water running out. Even after learning about this I would tell myself that there is just no way, I love pot too much and it helps the nausea so incredibly, there is just no way, the hot water has to help because my muscles are spazzing out or sore. This is what I have been telling myself for quite sometime.
Another thing that brings relief is running. No matter how many searches I do or where I look I can’t find anyone else that has the nausea relieved by running. Maybe I am shaking my guts up so they don’t have time to feel pain or discomfort. Needless to say the running isn’t ideal in the long run (no pun intended), it’s draining and counter productive because when going through one of these cycles it is nearly impossible to eat therefore one has no energy already to begin with.
Fast forward to today. For the past 3 days I have had this constant hunger feeling in the middle of my abdomen, it’s doesn’t even feel stomachy, feels like it is above my stomach. It is so extreme when I wake up in the morning I can’t even get any food down. A few times I have had to actually stand in the shower and eat a bowl of cereal…ridiculous I know. This particular time though I cannot fill the hunger void, no matter how much I eat, after 2 bananas and 3 bowls of cereal the feeling is still there, hunger, but more than that, a lot of pain as well. I know it isn’t a peptic ulcer, have been checked multiple times and I read that they can mimic hunger pains. So as I sit here typing this I have to just believe it’s from so much pot smoking. I mean I smoke a lot and always have, it makes sense. But it helps when I feel icky, a double edged sword we have here. I have stopped before to see if my symptoms might go away but I don’t think I was very honest with myself about it because I wanted to smoke, I feel like I really need to quit for about 5 to 6 months and see how i do for the next 2 or 3 months after that. So that’s what I am going to do. I know I probably rambled all throughout this post but I needed to get this out here, if not for me, for someone else suffering and denying the facts because they love to get stoned. It’s just not worth it, at this point I am starting to have problems in the bowel movement area (the receptors involved for cannibinoids also have to do with gastric motility )and I am losing so much weight, plus the toll it has taken on me mentally just makes everything worse. Living with this and smoking pot and being in denial will DESTROY your psyche…trust me.
Tammi, I wanted to ask you how your husband passed away exactly. Did his heart stop? Dehydrated and body just shut down? I am just curious what finally took him, and again my heart really does go out to you. Did your husband absolutely have to have pot in his times of despair, or just a hot shower? A lot of times it seems I need both, or at least the weed. Showers don’t cure it on their own anymore, maybe it has gotten that severe. I could sit here and type for hours about my history with this and the hell I have been through myself and my family. From ripping IV’s out of my arm at the hospital when discovering no pain medicine (in a cycle anti emetics do nothing, only pain meds will for some reason) would be administered, to multiple arguments and screaming matches with family members because of the frustration behind this. I would really like to talk more, eager to hear your reply.
-Rob
Tammy,
My husband suffers from CHS as well and i can’t begin to tell you how it’s affected all of our lives. I have been with him for 20 years and he has puked incessantly since the day I met him and been a VERY heavy marijuana user as well. He has been to every doctor, specialist you can think of. He’s been to the Cleveland Clinic , had every test possible and even had his gall bladder out. All they could tell us was Cyclic Vomiting Syndrome but no one knew the cause or could give him relief. No medicine would help …. just baths. So many hot baths that he would go through every towel in the house and it would go on for days when it was a bad bout. He would blame the sickness on something he ate, drank too much milk, ate too fast, etc etc. to say it’s been frustrating and maddening it has been for the last 20 years doesn’t even scratch the surface.
2 years ago a friend of mine who is a psychologist suggested all the pot might be making him sick… so I googled it and when I saw CHS come up I felt a great sense of relief … it was like I found the key to this we had been searching for all these years was finally in front of me and the cure was simple … all he has to do was stop smoking ! Simple right ? Nope. When I showed him my findings he told me I was out of my mind. That it wasn’t what he had… that I was crazy. I begged him to just stop for a few months and see what happens but he wouldn’t. My husband would smoke as soon as he woke up till he went to bed, every day for 20 years. Never a sober moment , I even begged him not to smoke before our wedding … couldn’t even do that for me. Every picture I have of him his eyes are glossed over..
So … after I found what I though was the cure he refused to believe it and continued to vomit every day like he has for 20 years before …. until he got arrested for DUAI drugs. A simple running of a stop sign changed everything. Officer smelled it in the car , did a sobriety test (which he failed) and found it in the car….. arrested! We are not people that get arrested! My husband is a suit, very well known in the community … I was humiliated. As part of his probation he was forced to do random drug testing … forced to quit. And low and behold… the vomiting immediately stopped. I couldn’t believe it … I felt validated. And he even let me give him the I told you so. It has been a little over a year now and he is off probation and started to smoke again but not to the degree he used to. I always know when he’s had too much because he starts puking again. I’ve given up begging him to stop. If he wants to continue to suffer then suffer.
I just hope it’s not too late for him… his teeth are so yellow from the acid coming up from his stomach it’s crazy , I also worry about throat cancer as well. This sickness has taken so much from us over the years …. practically every holiday or special occasion ruined because he was sick… missed school events , missed work, social events… even was sick for half our honeymoon. I hate to admit but I have no sympathy anymore for him … especially now that we know what is causing it. This sickness has driven a wedge between us and I feel resentment toward him when he gets sick, I just can’t help it. I am very sorry you lost your husband…. truly I am. I wish there was more education made available to the public and even doctors to help save people from suffering with this.
Tell him to take fiber everyday and exercise hot up a steam shower. We sufferers don’t process our toxins as easily. But he still needs to watch smoking in excess. Once he’s been continually taking the fiber he’ll be able to tell when e needs to slow down smoking if his BM’s become less and beginnings of constipation!
Taking fiber pills has helped me immensely. I think for us sufferers our body can’t process the toxins out as quickly so the more and more we smoke there more that gets built up. Which explains why hot showers(steam out toxins) running(sweating it out) help us. I’m 23 been smoking damn near everyday since I was 15. I started getting sick a few years ago which lead to multiple hospitals visits a year. Now in 2017; I had one hospital visit in all of 2016. So even though I take fiber and it helps, I can still over do it. Plan plan plan
If you want to smoke two blunts over the weekend you’ll have to take a few day break.
Take the fiber everyday; for me once I start feeling a little constipated I know it’s time for a cleanse.
So get rid of those toxins and keep smoking!!
Its scary. You think you’ll feel better but really you are making it worse. Then you cant tell if you are getting worse or having withdrawl or your body is just trying to hurt itself. Almost at a week into this and it wasn’t until the 3rd ER doctor saw me that he said it may be this. I had no idea. I was sensitive already to smells and perfumes and had bad morning sickness with my kids so all very scary and confusing. Once the ER doc gave me iv antibiotics (thinking could have been the bladder infection coming back) and that seemed to make me feel better, but every time they sent me home I would feel worse in the morning. I think it may be environmental too and could also be triggered through second and third hand smoke. I’m out the door for the weekend and will see if I feel better after a few days. I’m scared to eat and drink now because it all hurts. Im also on antibiotics, which I am not sure I need to be on and ER doc gave me T3 for the pain. Its such a helpless feeling but after the doc said could be this been trying to ‘flush’ the cannabinoids out of the fatty tissues and not sure how. Any ideas?
Tired hungry scared
Robert, I will start checking this every day to talk to you about this. Tami
This last week has been worst in my life. I’ve been dry heaving and puking all I drink. Just comes rite back up within minutes. Been to urgent care and the error. Five times in this last week. I have a high tolerance to weed so I would only smoke oils on the weed. Then last week I found RSO. After being on it for one day my stomach pain started and I’ve been sicker then a dog this hole time. The ER doctor on my last visit told me about this. Then he was very rude and wouldn’t help me at all. He told me to go home and suffer. Also I’m having trouble getting to sleep. And only sleeping an hour at a time. I’ve also been trying to lay on stomach to relieve the symptoms. Nothing helps. I can’t eat. All smells are gross. I’m for sure never going to smoke again. I had a very bad bone cancer. Plasma cytoma. Doctor took me off my pain pills because of pot. So I increased the pot and bam. This sucks. I’m actually been begging God to help me feel better.
Yeah fuck doctors against weed.
I was told to suffer many times as well
Taking fiber pills has helped me immensely. I think for us sufferers our body can’t process the toxins out as quickly so the more and more we smoke there more that gets built up. Which explains why hot showers(steam out toxins) running(sweating it out) help us. I’m 23 been smoking damn near everyday since I was 15. I started getting sick a few years ago which lead to multiple hospitals visits a year. Now in 2017; I had one hospital visit in all of 2016. So even though I take fiber and it helps, I can still over do it. Plan plan plan
If you want to smoke two blunts over the weekend you’ll have to take a few day break.
Take the fiber everyday; for me once I start feeling a little constipated I know it’s time for a cleanse.
So get rid of those toxins and keep smoking!!
How much fiber do you take to cleanse , I believe I’m in this mess too. Hard to admit it but I’ve tried everything and it all points to this
I’m still in denial. But at the same time I just don’t know. I wake up in the morning throwing up, anxiety in my chest, headaches, neaseous, I get the chills and start shaking. I don’t really shower for pain relief, I’ve done it twice and just end up puking in the shower. If I eat something at 9 pm and go to sleep at 3 am I wake up at 6 or 7 feelings horrible and throw up all morning.. I’ve been to the er about 5 times. The first time I went they said I had an inflamed intestine and some colitis and that my white cells were high. They gave me antibiotics, and for neasea . Nothing helped. So I kept going back to the er, they would put me on ativan and iv then would send me home. The last time I went the doctor he said that there is nothing they can do and that they found weed in my blood and he was certain that CHS is my problem. That was about a month ago. I started feeling better after 3 days and started smoking again. Month later I’m waking up in the morning again puking my brains out. I keep telling myself not to smoke but can’t help it since it really does make me feel better! I feel lost and stuck. My husband takes care of me when he’s here but he works all day everyday so I’m mostly home alone and it’s just a lot :*( also to make things worse, I just got my period and I feel so sick. I just want to die.
Taking fiber pills has helped me immensely. I think for us sufferers our body can’t process the toxins out as quickly so the more and more we smoke there more that gets built up. Which explains why hot showers(steam out toxins) running(sweating it out) help us. I’m 23 been smoking damn near everyday since I was 15. I started getting sick a few years ago which lead to multiple hospitals visits a year. Now in 2017; I had one hospital visit in all of 2016. So even though I take fiber and it helps, I can still over do it. Plan plan plan
If you want to smoke two blunts over the weekend you’ll have to take a few day break.
Take the fiber everyday; for me once I start feeling a little constipated I know it’s time for a cleanse.
So get rid of those toxins and keep smoking!!
*be careful around periods they are bad for me mostly from excess dehydration
Good luck!
Are there any studies being done on this …. so i was a pot smoker daily for roughly 15 yrs… then the sickness started … after three yrs of racking up er bills and gallbladder removal a nurse said off the record that she would bet me money this was my problem… so i quit …felt so out of place for a while dealing with sleep issues and anxieties… even night sweats but after a month i was getting normal …. 2 sober yrs later i decided to try a little pot but only in moderation … 2 months later sick again… i love pot but appareantly a section of my brain doesnt… i would participate in some studies if there any dealing with this
Jab,
We are not aware of any such studies but if we do, we will contact you immediately.
Best,
Mary Ann
Taking fiber pills has helped me immensely. I think for us sufferers our body can’t process the toxins out as quickly so the more and more we smoke there more that gets built up. Which explains why hot showers(steam out toxins) running(sweating it out) help us. I’m 23 been smoking damn near everyday since I was 15. I started getting sick a few years ago which lead to multiple hospitals visits a year. Now in 2017; I had one hospital visit in all of 2016. So even though I take fiber and it helps, I can still over do it. Plan plan plan
If you want to smoke two blunts over the weekend you’ll have to take a few day break.
Take the fiber everyday; for me once I start feeling a little constipated I know it’s time for a cleanse.
So get rid of those toxins and keep smoking!!
Hello all-
My husband just went to the er after 5 bouts (that we can recall) this year of extreme vomiting and cold chills coupled with sweating and weakness all over – only thing that ever helped was hot water – mostly showers- and of course smoking more. We were about to go down the tract of upper gi testing etc. when the er doc told us about this – we had NEVER heard of such a syndrome and were in disbelief – we searched and found several descriptions of exactly what he has been experiencing – he is a classic case…. We are so glad to get to the bottom of this cyclical syndrome…. He has been a daily heavy user for 30 years – it’s scary to think of quitting but he is certain that is the only choice.. He missed Father’s Day- first day of beach vacation in August and just spent two days sick while camping 6 hours from home on a beautifully planned trip to the ocean… ENOUGH!!
I’m a 22 year old female and I have smoked multiple times daily since I was 17. I thought it was helping me from being nauseas in the mornings, but instead of helping me it ended up hurting me. I would have swore by weed as a miracle a week ago, now I will never touch my beloved friend again. I have had over ten Emergency visits to the hospital within a year. Many diagnostic tests such as CT scans, ultrasounds, and even a HIDA scan on my gall bladder, but nothing unusual except for some enzyme levels up which I now believe must have been triggered by a chemical the weed was grown with. Other than that my insides are perfectly normal and functional. I would have nausea and retching that lasted hours and days, mainly in the mornings. The pain was so bad that morphine did nothing for me, and there was not a single nausea medicine that helped. Dilaudid would only help but not for too long. I now am 5′ 7″ and weigh 85 pounds after dropping so much weight within the last year. I haven’t smoked in exactly a week and I have not woken up a single morning in pain or nauseas. I was very reluctant to believe my nurses when they told me of this syndrome but I know without a shadow of a doubt that weed was making me sick. I still believe that medical marijuana is a great thing for many people, and honestly I think it’s fine for people to use recreationally as long as they aren’t suffering from these symptoms. I never thought I could break the habit nor did I want to give up my best girl Mary Jane, but I just can’t help but think the chemicals weed is grown with today are no good for the human body. I don’t think this wil effect many people, but I was just a susceptible person with an already weak body. With that being said I’m sure there are many others out there dealing with the same thing who maybe don’t realize it. I know it’s hard but if you quit smoking it wil get better, and you will actually feel better than how you felt puking every morning while trying to smoke. All of my symptoms have know gone and I wil never hang out with Mary Jane again. I hope she’s a great best friend for someone else.
My son had been admitted to a hospital after going to ER. 3 times in the last 30 days. The last time a dr recognized his symptoms and told us of CHS. He has also the symptoms especially the hot baths. He would come home to my house after he ran out if hot water at his house. Then go smoke a one hitter to make it feel better only to get sick again. He was first diagnosed with CVs a few years ago. He started smoking weed in high school and started to get sick at 18. Now 13 years later he might have a chance to live again. He has lost jobs and girlfriends and most of all he lost alot of his youth in a bathtub. As his Mother it has been very frustrating. We would get angry with each other when he had his episodes. I felt guilty about this and I got to the point was where I didn’t want to take him to the ER because I knew it was a bag or 2 of fluids , maybe some anti nausea meds and out the door. This has cost him thousands of dollars. Can anyone tell me how long the hospital stay will be for him? It has been 24 hours now and he is improving.
Please Help me understand how as a family member I can help him
In my last comment I stated it has been 24 hours and he is improving. Typo. He is NOT.
I am 22 years old. Been smoking pot everyday, multiple times a day since I was 15. Didn’t feel any symptoms for years. Around the age of 19, every time I drank alcohol I would puke dozens of times, all day, for a week straight, usually. So I kicked alcohol but kept smoking regularly. Didn’t have an episode until 6 months later, and boy was I shocked. I figured, I had stopped drinking, what could this be from now?? Same thing happened, nausea, abdominal pain, cyclic vomitting for days, no food or drinks, the chills, sweat, and weight loss, dizziness, excessive thirst only to throw anything up, retching, slow bowel movement ect. then my esophagus gets in this sharp pain due to the vomitting. That’s when I take scolding hot showers, they make it slightly bearable but still I end up sick. When I heard about this CHS i thought no way, all my friends are stoners, they would have this too! but after doing some research it seemed there was no other explanation. They diagnosed me with cyclic vomitting syndrome at first, but then once it happened another 6mo later, they finally thought of CHS. I keep getting sick because I have the hardest time not smoking weed. My last episode was October 6th. And I’m still recovering from the nausea and esophagus pain. It’s probably because when I got out of the hospital I smoked again :( (not smart). Before this, my last episode was 6mos before that and so on and so forth. I am one week into not smoking tobacco or weed and I’m still in pain but I’m trying very hard to sustain from smoking. Ironically, I got a pot card today to find alternatives to smoking weed, but I am fearful now that the same thing can happen from edibles and tinctures. From the research I have done, it seems to have something to do with the CB receptors. But I really don’t understand chemical stuff :/ I’m terrified that this could turn into some sort of cancer or ulcer! Does anyone have any advise or new knowledge that may be helpful?
Started happening to me a few years ago. I still occasionally get sick if I don’t watch how much I smoke.
But my answer has been FIBER!!
That’s right! I’m 23 and take fiber 4 times a day everyday and it has helped immensely. Once I start feeling constipated while taking fiber. I know it’s time to take a couple day break to get the toxins out.
Basically I think all this excess smoke just isn’t able to process fast enough in some of us.
Hope this helps!! I still smoke everyday now. Just remember not to smoke tooo much
I’m a 27 yr old male who had been dealing with cyclic vomiting episodes for the past 10 years, about as long as I have been a daily marijuana user, starting out recreationally and mostly now for nausea(or so I thought). I was 19 when i had my first episode, this is where i discovered about the hot showers being a help, along with smoking. I live in a small town and after all the tests they were stumped, I was sent to another doctor and when I mentioned hot showers, he diagnosed me with CVS or cyclic vomiting syndrome. I went a couple years, still smoking, mostly symptom free using all the meds he gave me. My episodes returned and my local gi doctor brought up CHS. I was skeptical and dismissed it. But after a recent bout of episodes that put my job in jeopardy along with research I am almost POSITIVE I have CHS. Because I kno hot showers and weed can help in the short term, i haven’t had to go to the ER but il also go 3-4 days dry heaving and only sipping water here and there. I have recently spent over 3000$ getting a colonoscopy and a gi scope, with other tests and I’m healthy, they said I had IBS because I said I had stopped smoking, just so they would go on and test me. No answers for my episodes so I have to believe this is it. 2 years ago I quit for 2 months for my job and my nausea went away, I started up casually and nausea and vomiting episodes returned. After researching today, I have to admit to myself that this has to be it….some of my symptoms similar to others who came to this conclusion include
Every day marijuana use
Hot showers help with symptoms
Waking up in the morning vomiting
Abdominal pain/ bowel movement changes
Episodes last 1-4 days usually 2-3 times a year
Diagnosed with CVS
Hope this helps as the prior posts helped me conclude that I need to make changes in life and smoking marijuana can’t be one of them, no matter how much it helps in the short term it makes too much sense for it not to be what’s making me sick. Save your money because not one doctor in my town suggested this to me!!
Taking fiber pills has helped me immensely. I think for us sufferers our body can’t process the toxins out as quickly so the more and more we smoke there more that gets built up. Which explains why hot showers(steam out toxins) running(sweating it out) help us. I’m 23 been smoking damn near everyday since I was 15. I started getting sick a few years ago which lead to multiple hospitals visits a year. Now in 2017; I had one hospital visit in all of 2016. So even though I take fiber and it helps, I can still over do it. Plan plan plan
If you want to smoke two blunts over the weekend you’ll have to take a few day break.
Take the fiber everyday; for me once I start feeling a little constipated I know it’s time for a cleanse.
So get rid of those toxins and keep smoking!!
I have also been diagnosed with cannabis hyperemesis. I actually ended up in the hospital twice because of it. Whenever it happened I would throw up for a week or two, constantly and couldn’t hold any food down. I lost a lot of weight and was super dehydrated. The only cure for it is really to stop smoking, or smoke in a way that doesn’t cause it to act up again. My advice is to quit completely if you can, but if you must smoke, do it rarely. I have found that if I don’t smoke every single day I feel totally fine. I used to smoke every day for years, multiple times a day. Now I do it only a couple times a week, or if I do for a full week, I will take another week break before I do it again. You just have to find what works for you.
I’m so happy to have found this article… CHS is something, as a pot smoker, I would have scoffed at a year and a half ago.
But about a year and a half ago, my youngest daughter started having symptoms that her older sister started having 9 years prior. Sudden, brutal, debilitating vomiting and abdominal pain that is only relieved by scalding hot showers/baths. The vomit in both girls was always pure yellow. Nothing but pure yellow fluid. The bouts lasted between 7-9 days. Dehydration and hospital visits numbered in the dozens over a period of a few months. Gall bladder removal surgery for the youngest daughter. Which solved nothing. Specialists, invasive testing, lost wages, lost weight, and lost jobs. Life as our family knew it was obliterated.
Finally, by process of elimination and over a year since onset, the youngest of my two daughters was diagnosed with CHS. She quit smoking immediately. At that point she was so sick, so often (about 40% of the time) that quitting was a no brainer.
It’s been three and a half months and she has not had a single episode of vomiting since quitting. To put it in perspective, she had not gone more than 14 days between recovery and the next outbreak in over a year prior to quitting.
My oldest daughter was so sick that I had to assume guardianship of my grand daughter. She was just released from the hospital today after a four day rehydration session. She has also now been diagnosed with CHS.
Believe me, this IS real.
I was diagnosed December 23rd 2015 with CHS after over two and a half years of not knowing the real problem. Much like everyone else I had CT scans, endoscope, tests upon tests, with no results. We even thought it was gallstones for a while. In one year alone I had 19 ER visits. The pain, nausea, and vomiting would last hours. I kept smoking more, thinking marijuana is an antiemetic, so it has to be helping with the nausea. Little did I know it was just adding to the problem.
I wish there was a way to inform more people about this syndrome, and have it be studied. I love marijuana and am saddened I cannot consume it like I have in the past. Most people (much like myself) when I first tell them don’t believe me and think I am saying these things because I am anti-marijuana, which is not the case at all.
I could go on and on about this sickness, but I am just happy to have found answers before it was too late. I was very skinny and very unwell when I was diagnosed, so I am very lucky I found out.
Not one doctor in Manitoba knew about the syndrome, hence my constant ER visits. All it took was one ER visit in Ontario (was visiting people in Thunder Bay) and the doctor knew right away my problem. I of course had denial about it but after reading a lot on the internet, paired with sessation, I got better in time. It took a bit of time, and I went through hellish withdrawals.
Hopefully as the world progresses so will the knowledge and information on this syndrome.
The solution is stopped smoking weed and you’ll get better in no time!!
Their are a few things I think that should be said about chs that I saw happen in my husband sickness. First, his brother and friend smoked the same pot and just as much,even worked together. They have never been sick,to this day and they have smoked for 45 years.Another thing to remember is at first there could be a few years that he wouldn’t be sick and then as the years went on,it was more often. He was found dead sitting on the floor of the shower. When the autopsy was done,there was NO organ failure and after the second one was done there was no answer why. He didn’t know he was going to die. After all these years (25) and seeing all he missed out on,it makes me sick even writing this.I remember Erica,all the times that were ruined because he was sick,but I didn’t know why.I can’t believe he missed his two son lives their wives and 8 grandchildren for smoking pot.
Does anyone know how long it could take to stop the nausea and vomiting? My daughter has been in the hospital for 2 weeks and her symptoms have not really improved. She has been diagnosed with Gastroparesis but now they say its chronic small bowel dysmotility so I don’t know if it has moved from her stomach down or what because the barium swallow test that took 5 hours said the barium moved fine through her stomach. She has been dealing with this for 3 years to the point she has a feeding tube! She did have stomach issues when she was 14 and has always been thin and never much of an appetite but her Sophomore year in college she had another episode and every 6 months after that until 3 years ago. She started smoking daily/ multiple times a day after her Sophomore year in college and even did the dab stuff for a long time. Right now she has stopped for the two weeks she has been in the hospital. We brought it to the doctor’s attention and they are glad she is going to quit but they are basically discounting it as the issue. I wanted them to try the Haldol while she is in the hospital (that some here and other places say works to knock the nausea and vomiting and pain out) but they don’t want to try it! The IV Phenergan is so hard on her veins and it doesn’t even help that much. The dilaudid helps but I don’t want to trade one problem for another – she gets the meds every time she can and sometimes the vomiting happens anyway. Zofran and Morphine don’t phase her.
Any other meds or suggestions? She is unable to take the hot showers because she just had her feeding tube replaced.
Thanks!
Hello Ms. Stone,
From your note it sounds like your daughter was not diagnosed with Hypermesis. It sounded like her symptoms subsided when she was smoking if I understand this correctly.
Cannabis, in the proper formulation, can work very well for nausea and pharmaceuticals are rarely needed when appoaching this from medical standpoint.
We have medical staff that offer consutlations online or via skype if you are interested. I am adding the link to the scheduling system here for your convenience.
Of course, where you live will dictate your ability to attain the correct cannabis medicine as some states and counties still have a ban on the medicine at this time.
I hope this helps!
Mary Ann
Look into thyroid. Long story to sum it all up. It wont allow her to keep smoking pot, but it will help her. Free t3 is the test you want, or, better yet, waking temp and pulse. Tsh has notbing to do with cellular thyroid acticity. Not to sound 12-stepy, but for others here, getting on thyroid has taken away my need for weed. Weed was a cheap substitute compared to thyroid, and almost all people need it. Check 9ut ray peat. Hope your daughter gets better soon.
Hi there. My name is Taylor, I’m 21 years old, and I’ve been to the ER three times in the past 2 weeks for excessive vommitting, dehydration, and severe abdominal pain. (My pain level was so bad that my screaming in the ER waiting room was scaring the other people) when the vommitting started I assumed it was just a bad case of the stomach flu, as I was hospitalized for that twice this year. But as the days went on and nothing was getting better and the pain continued to get worse I went into the ER. I was there for 12 hours. They ran multiple tests and an ultrasound and eventually diagnosed it as a peptic ulcer where I would take sold ran for nausea and Pepcid twice daily. Well, three days later my symptoms only got worse and lo and behold, I was in the ER again, but this time the pain was INTOLERABLE. my mom raised me to be tough as nails but I couldn’t even contain the sounds that were coming from me. I’ve never had such pain in my life. My body was constantly trying to expell stuff in my stomach even though there was nothing left in there. I would just choke and gag on my own bile spit. They administered morphine and benzos via IV which gave me more relief than I had in days. But the doctor treating me this time was completely different. Last time I went in I was open and honest about my cannabis use (I have severe endometriosis so I love with constant painful cramping and a Lott of back pain, and migraines every day. I was on narcotics for 4 years before my boyfriend had me try marijuana to help alleviate my symptoms. Needless to say I completely switched over as I’m only 21 and don’t want to be addicted to narcotics. I smoke what’s known as ‘dabs’ as its a more controlled high for me with more pain relief) and he wasn’t judgmental and gave me the best treatment possible. This time around I was treated like a junkie, for lack of better words. The doctor told me I had cannabis hypermesis and would suffer for the next few weeks. She wouldn’t allow my parents in the room as she explained this to me and continually propped me about my sexual history for some reason. (Mind you I’ve had the same partner for 2 years and we both get tested regularly) After she explained her diagnosis I was basically kicked out of the ER. I as still in excruciating pain when I left and as I was waiting outside for my father to bring the car around, a nurse walking by even asked if I needed to be wheeled in and checked in. Well, I a, now going on two weeks of the symptoms. My sleeping schedule is fucked, my hair is falling out, and where I was once a healthy, curvy 132lb woman, I now weigh a measly 98lb’s and can barely hold down chicken broth. I get so exhausted from the tiniest things and I feel depressed and anxious all the time. My parents had me at their apartment for a week, but with two younger siblings I was becoming a burden. I’m back home with my boyfriend who is an absolute angel, but is working overtime just to pay for my medical bills, prescriptions,and make rent so we have a place to live. I have 6 other roommates who aren’t very clean people and only a shower. No bathtub. Baths provided relief for me but sitting in the shower I just feel exhausted and sad. I am trying so hard to stay strong and get through this, but each time I think I’m tUrning a corner, things just get worse and I start vommitting or writhing in pain. All I want is to get better. I will try anything at this point, I am just so miserable and it’s affecting the people I love and I can’t stand it. Any prayers, any advice, any help at all is appreciated more than you know. Thank you so much.
Heartbreaking. Dessicated thyroid and/or progestero e in vitamin e shohld fix you up.
I am 23 years old and had this CHS symptoms for about 3 years before i found out that it was and what was CHS. Showers is where I found most of my relief from. Correction scalding hot showers. I’ve been in the hospital twice and also on one occasion I stayed home. This is very serious and real. I have quit smoking pot for 6 months now and I have not had one sign of the symptoms at all. Just quitting is the answer until further research is done. I have been wanting to smoke again maybe just one but that always leads to more. I would love to be part of some research as well as writing articles on this subject. I know I can speak for most people who’ve gone through this and say they would have love to continue smoking pot. I never knew this would be possible or even come to this from smoking weed. Hopefully one day they can figure out the answer or maybe find an alternative. I now watch my friends enjoy smoking and my girlfriend enjoy smoking and I would love to just hit it a few times but then I think back for me being in the hospital for 10 days constantly being sick also 2 years ago how sick I was. I also remember the sickness feeling in the morning. I also lost a job offer from waking up one morning and getting very very sick on my first day. Please keep me informed on any studies that will be or possibly conducted. I would like to be a part of it to finding some solution for all pot lovers. For now I’m just going to continue to be sober and get my life in line and hopefully at the end of my retirement stage I can enjoy smoking on my front porch looking over my farm.
I started smoking at 16. Very heavily up until about 31. I have been to the ER more than 20 times, admitted many of those times, and even to Johns Hopkins once to get some answers. My last bout was exactly one week ago. The usual. In the ER, admitted, out the next day. The next morning BAM again. To the ER and after my usual IVs, zofran, and 3 doses of dilauded I felt better. Then the doctor tells me about hcs. 19 years it took to get that answer…
I am an alcoholic with almost 3 years sobriety. I have abused both pot and alcohol to the extreme. Consequences from pot – zero
Consequences from alcohol – lost job, lost fiancée, lost house, two Dui’s, and so many more I can’t even list them. The reason I say this is because pot is so much better and safer then alcohol. I am a huge advocate of marijuana. So too anyone who says we are just haters, we are not. We are just the unlucky few. But I write this because chs ruined many, many days/months for me. From 19-31 I was in and out of the ER more times than I care to remember. I was taking hot baths at 19. No idea why but it seemed to help. I knew dilauded and benzos helped at 20. Anti nausea medicine did nothing. I would beg ER docs for dilauded but well, you know how that goes… I would suffer for days while they ran all kinds of test on me. This happened again just last week on my first visit. Despite me saying all I needed was dilauded, they didn’t give it to me while they ran Ct scans, ultrasounds, blood work,etc while I suffered. how many times this was the case for me, 9 out of 10. I could only hope and pray that I got that one doc who was cool and just wanted to take away my suffering. This has been my entire life. Johns Hopkins told me one thing – don’t drink alcohol. I was 20 then. I barely ever drank back then. Marijuana was always my choice. I didn’t even like alcohol. I did not drink alcohol my entire 20’s. I loved pot! I was diagnosed with GERD at 21 after a boute and until last week I always thought that was my problem. I have taken Prevacid every day since. But after the doc told me last week about chs I started doing research and OMG. There it is. All this time. I did not smoke from 31-34 because I was on probation for my Dui’s. not once in that time did I have an episode. But a couple months ago when I got off probation I started smoking again. I have a sponsor, attend AA regularly, and my sobriety was stronger than ever. And still is. But sure enough after smoking daily for 3 months, it struck again. Now that I know what the cause is, I will no longer smoke. Yes, for me it is that simple but only because battling alcoholism was the hardest thing I’ve ever done in my life and frankly after that, quitting pot is a piece of cake. Would I like to smoke? Hell yeah. But not at that price. I also knew the whole time I was smoking these past 3 months that I wasn’t being my “best self”. Hell, weed is great. But a sober me is always a better me, No matter how little the better may be. To put it in numbers: a drinking me is a 2/10, a terrible human being. A smoking me is a 9/10, a good man but still not the best me. Hey, I’m cool with 9/10. But again, not at the price of endless pain, endless nausea, endless hospital bills, and the toll it takes on family/friends/work etc…
I have never posted on any site, ever. This is the first time. Why? Because I want to help!!! As marijuana becomes more legal, chs will become more well known and much more common. We need studies and research. I want to help. I’m not saying I want to smoke again, but I feel my experiences can help others. If there are any medical professionals looking into this, I want to help. If u r someone who suffers from this, I want to help. Life is good, god is great, and I am truly blessed for all he has given me. Chs sucks, but what really sucks is the absolute lack of knowledge about it. How can so many medical professionals over the years not know about this? It’s time to get this mainstream so the thousands out there suffering don’t have to.
I am 35, have a great job, a wonderful daughter, and if u met me on the street would never guess I am an alcoholic or avid pot smoker. I say this because it can happen to anyone.
I want to help.
I give this site permission to share my email with medical professionals who are looking for help. I want to help.
To finish, I will say this. If u r suffering, the next time you go to the hospital, tell your doctor about chs. Sadly enough, it may be the first they have heard about it. But it also may save you hours of unneeded pain and suffering. Dilauded and benzos. Of course iv fluids too. But dilauded and benzos are they instant relief answer.
God bless.
When i see im not the only one with these horrible problems (no one understands unless you go through it I promise) it makes me feel a lil better…IM NOT SAYING THIS WILL WORK FOR EVERYONE BUT I Partially CURED MYSELF..and heres how..Ok so my symptoms started my 3rd year in college after smoking literally multiple blunts a day for 3 years..my 3rd year was the worst time of my life, i dropped out of college because of this problem and yes its that real. I could never stay sleep my nausea and vomiting woke me up every morning. But after i came back home from college i had stopped for maybe 2months and within those 2 months i got back in good shape and ate pretty healthy. I started back smoking now and havent threw up since, i will sometimes wake up with nausea but i smoke and feel better but overall no throwing up anymore…So heres my tip for anyone, try getting A work-out plan and smoke after you work out..just stopping isn’t that easy as people think specially when whats causing the problem is what also makes us feel better…I promise no one will understand these problems unless you experience it good luck my fellow stoners…
I was diagnosed with CHS on vacation last week in Colorado. I am a 20 year old male but only smoke 2-3 times per week. I don’t seem to fit the typical heavy marijuana user that then has CHS. Could I have been misdiagnosed? Last time I smoked was 6 days ago and I am still having the extreme nausea but not vomiting very often. At this point I can only drink water and gatorade, no food.
The ER doctor told me he was 100% I have CHS and that in Colorado they are seeing 50+ cases a day across the state in ER rooms.
If I do have CHS how much longer will the nausea last??? Does it really take 2 weeks from the last time I smoked???
Hey, I just read the whole comment section; I never knew this was such an issue and as someone else here said I wouldn’t of even believed this was real a few weeks ago.
I’ve now been in the hospital for 8 days with severe nausea everyone I eat or drink anything. I have been a frequent cannabis user for years although I don’t smoke, I strictly used edibles. My question is the following: how long is this supposed to last? Is it supposed to be upwards of a week? Has anyone found any sort of cure or had success with their hospital treatment?
Thank you to anyone who replies, any help is appreciated.
Oscar, mine lasted for roughly a week. If youre still in the hospital, have them put you on Lorazepam. Once youre out, talk to the dr about a prescription for metoclopramide to help restore stomach function so you can start eating again. Feel free to contact me any time, Ive been fighting this for 8 years.
Alan-
The symptoms can last two weeks to a month. It’s a slow process. And the kidney function is what tend to take the longest to relieve. Drinking excessive water (as much as you can), soup broth, and crackers have helped me before. Best of luck to all.
Pretty sure we are going to see an avalanche on this site. Excellent work moderators, I learned a lot.
I’ve had this for decades, puzzled all but one old GI Doc who dimly remembered an article about hot showers.
Even with this tip, it too me another couple of years to really figure this out.
On a lot of sites, people are really fighting back against this. If you have it,, you know it. If you don’t have it, you really don’t have a clue.
I have been searching for days for a single person who has really been able to use and not be sick. People seem to have tried almost everything.
For some reason I can’t get on his site to leave a message, but if someone could tell the moron who thinks this is a “Az” organic pesticides, he is completely out to lunch. I grow, or grew I guess I should say, 100% organic and don’t even use root hormone. Not one single additive of anykind. Compost and sunlight and water. Thats it. He is giving people a lot of false hope.
I’m sorry but I think its quitsville for this pothead. Some better advice on alieving the withdrawals would be helpful.
add my name to those willing to discuss with doctors/researchers.
Hey, I’m making another post to see if anyone can 100% confirm that I have CVS as my doctors think I do, and I think I do; however you can never be to sure.
I have been in the hospital for 12 days. I am now able to drink liquids as of 3 days ago and some soup, occasionally however I still vomit it out. Something like orange juice would be enough to have me puking. I don’t understand how anyone suffering from this would be able to live let alone work, if I wasn’t at the hospital all this time surely I’d be dead. Are my symptoms CVS? Or do they just match enough for a diagnosis? I’ve had an endoscopy and many CT scans to no avail. Thank you to anyone who can shed some light, I’m just looking for the opinions of those who have gone through this there really isn’t much information out there at all.
Oscar,
Did the cananbis that you ingested come with test results. Typically CVS doesn’t last days and can be remedied with a hot shower. Your symptoms would make us wonder if their were toxins or pesticides in your canabis.
Just a thought,
UPG
I am a quadriplegic and have used medical marijuana daily to help with pain. I was using Percocet 3-4 times a day but stopped when I started medical marijuana a year ago. I figured marijuana was way better than opioids for the long term. I’ve used medical marijuana multiple times a day for over a year. I don’t vomit but have felt a little nausea lately. I do have some feeling below my level of injury and lately have felt crampy in my stomach. It may just be a bug. But I’ve stopped taking medical marijuana for 2 days now out of fear. Should I stop permanently so I don’t get Cannabinoid Hyperemesis Syndrome? The last year has been great. I’ve been extremely productive and successful. I’ve ran 2 businesses. The medical marijuana doesn’t always take the pain away but it’s helped me through it. Will I eventually develop Cannabinoid Hyperemesis Syndrome if I continue to use?
UPG Staff–CVS isn’t CHS…duh…and CHS can’t be “remedied with a hot shower”
Its not a remedy, its stop gap coping mechanism that will soon not work.
Pesticides in weed, NO WAY it causes 15 days in hospital.
Is there a one post limit? Cause I sought to include more advice as I go through this process, but I’m not seeing it here.
Can you please PM me if you choose not to post this?
Thanks,
Concerned.
Christopher,
If you’d like to write a blog on this topic we are happy to post it. As long as the content is respectful and includes sources, not opinion, we are always open for public offerings.
UPG Staff
Here’s a little twist. Maybe it will help find an answer. I’ve been having severe nausea and vomiting for at least a year. I am a long time, chronic smoker and this diagnosis fits perfectly. After crazy amounts of testing and doctors visits, nothing but despair. I thought it was a food allergy, celiac or a sugar issue but all testing shows negative. Just nausea and vomiting from anywhere from 1 hour to 24 hours in duration. Constant retching shows up sometimes, usually the longer duration sessions. It’s intermittent and always starts after eating out at a restaurant.
Why do I only get sick when i go out? Anxiety, Stress?? It doesn’t happen every time and doesn’t happen at home. Makes for a tough vacation. I don’t have the urge for the hot water but I’m definitely going to try next time.
https://thecleangame.net/2015/12/cannabis-hyperemesis-actually-azadirachtin-poisoning/
Just try taking fiber daily!!!
Still have to be cautious about smoking in excess.
Plan plan plan
If you want to smoke two blunts on the weekend take a few day cleanse while keeping up with the fiber.
When taking fiber if you Begin to have fewer BM’s and start of constipation it’s time for a complete body cleanse stop for a week or more and sweat out those toxins!!
Good luck!!
My story is very long and promise I will tell the whole thing one day so for now heres a quick outline and relief for anyone currently in the hospital looking for help!!
-started smoking in 2001 at the age of 17
-used intermittently for 2 years(couple times a week for a few months, then would quit for a few months)
-began heavy use(multiple times a day for 8 months, quit for 2 months, then resumed heavy consumption
-experienced my first episode of cyclic vomiting in 2008
-after 10 days of non-stop vomiting, I suffered acute Renal failure(kidney failure)
-this led to my 1st misdiagnosis – IgM Nephropathy
-released from the hospital 1 week later after treatment for renal failure
-marijuana consumption ceased for approximately 1 year
-all symptoms ceased except for a delay in gastric emptying
-this was my 2nd misdiagnosis – Sluggish Stomach Disease and Lactose Intolerance
-over the next 2 years, i smoked marijuana intermittently
-2011 i suffered another bout of cyclic vomiting and a 2nd round of Renal failure
-this led to my 3rd misdiagnosis – Minimal Change Disease
-intermittent marijuana usage continued over the next 5 years
-i would quit smoking frequently enough not to have these vomiting bouts and renal failure
-March 2016 i suffered my 3rd occurrence of renal failure
-this led to my most recent diagnosis – Cyclic Vomiting Syndrome(CVS)
– I have ceased all marijuana usage after learning it aggravates CVS and have had no vomiting since but still have remnants of slow gastric emptying
During all of this, HOT SHOWERS were the only thing that provided relief.
MEDS
During vomiting episodes – LORAZEPAM, LORAZEPAM, LORAZEPAM!!!!
After vomiting subsides, what worked for me to re-introduce food was to start with a liquid diet of apple juice, then introduce apple sauce, finally regular solid foods
Extended-use medicine to treat gastric emptying is Metoclopromide 10mg
The Lorazepam stops the vomiting, the Metoclopromide helps stomach function. I have tried dozens of other meds but they are not important as they did not help.
ANYONE is welcome to contact me and I will be more than happy to talk to you and help in any way possible, I will email, text, talk on the phone, video chat, whatever you need. It took me 8 years to finally get the right answers and I dont want anyone else to suffer for that long. If you are a marijuana user, just like me, you have to get over your denial. This sucks, I know. I prefer to smoke over drinking. It is much much safer but some of us are just not lucky and it effects us in a negative fashion. Stopping smoking is the only thing that will stop these vomiting bouts from happening. Please, PLEASE do not hesitate to contact me!
Steve T
acnstnj@hotmail.com
I must chime in here. (long)
I experienced chronic nausea and vomiting for nearly a year when I was 10-11 years old and was starting puberty. (At that time I had tried cannabis a couple times, and alcohol too, but nothing excessive or regular.) The symptoms subsided on their own without any lifestyle/dietary changes. I don’t blame the symptoms on cannabis. At age 13 when I began using cannabis every chance I could, which was about twice a week or so up until age 17, I didn’t experience any symptoms or negative effects whatsoever. Only the positive effects we all love so much.
Right before age 18 I began dealing and using cannabis several times daily, and the nausea/vomiting symptoms I had experienced years ago returned. I had always read about how cannabis was used to treat nausea so of course I began using more. This led me to believe I had an underlying condition which manifested when I was younger, and had now returned. The nausea/vomiting would come and go, seemingly at random, sometimes for an hour, a day, or weeks/months at a time, and sometimes I’d be symptom free for months. I’d blame diet, stress, or some underlying illness I had or contracted. The symptoms seemed to get worse as I grew older, even though I tended to consume less cannabis, but was still a regular user, 2-4 times a day, about 1-2 grams total daily. I never went more than 1 day without cannabis. I was a daily user, skipping 2-3 days per year.
I had gone to many doctors/specialists and had many tests done, which always came back normal, aside from some high/low good/bad cholesterol levels, and some hormone levels too low. Until age 30 when I began seeing a very expensive gastroenterologist, I had an ultrasound of my liver which revealed fatty liver disease. I immediately changed my diet by cutting out dairy and limiting sugar (I would consume 4-6 sodas/sweet teas daily). I was also overweight and was losing my hair. I cut out high fructose corn syrup and hydrogenated oil, and limited slow digesting foods, and stopped eating before bedtime. This helped a little and I lost about 20 pounds, got down to normal weight. Stress and social situations seemed to trigger symptoms. I always felt worse after eating, had trouble falling asleep, and was very sensitive to cold weather. (never correlated relief with hot showers/baths until I began reading about hyperemesis syndrome, but I definitely experienced it.)
At age 32 I took a break from using cannabis for about 2 months and my condition seemed to improve, less severe symptoms happening less often, but still had symptoms. Mostly lower digestive, cramping and diarrhea, not so much nausea vomiting.
At age 33 I went to prison for 2 years and did not consume any cannabis whatsoever. I still had symptoms, but they were remarkably less severe and happened less often, even under the stressful prison environment and the shitty food being served. In prison I’d have bowel movements about once or twice per week. At home was once or twice per day, sometimes more, and I had lots of painful cramping and diarrhea with undigested food.
Upon being released from prison, I began using cannabis again almost immediately. About a month after being released, I smoked heavily for a few days and became very ill for about a week, not able to eat or get out of bed except to use the restroom with explosive diarrhea.
I’m now 42 years old. My symptoms have been consistent when I would smoke; nausea, vomiting, diarrhea, intestinal cramping, heartburn, chills, weakness, fatigue, burning stomach which feels like starvation, general flu-like symptoms. I’ve tried vaporizing and edibles, with severe symptoms from edibles, and next-day symptoms from vaporizing lasting several days afterwards. I’ll also point out that historically my delivery method of choice was always waterpipes/bongs, until a few years ago I used small pipes and joints exclusively.
I believe this syndrome to be very real. I haven’t consumed any cannabis in about a week and I feel 80% better. For a period of time before I went to prison, I had almost exclusively consumed a single variety of cannabis (Jack Herer) that I personally grew myself without any pesticides. I grew a large batch with chemical hydroponics and a small patch in organic soil. The symptoms seemed to be less severe with the organic, but still present. (could be psychological) Some varieties I’d consume from other growers produced no immediate symptoms. Indicas seemed to produce less severe symptoms than sativas, or no symptoms, but honestly it’s difficult to know exactly because of the nature of this syndrome.
I’ve decided I’m going to take a very long break from cannabis, perhaps even quitting altogether. I’m typing this with tears rolling down my cheeks. I’ve fought and sacrificed a whole lot in favor of legalization, and it makes me happy to see that happening across the country. I will continue to be an advocate for legalization of both medical and recreational cannabis, and to end the drug war altogether. Eventually I’d like to see the entire government abolished, but that’s a discussion we can have another day.
Thank you for reading.
Sincerely,
J
UPDATE
Just got out of hospital, collapsed with chess pains, ambulance. Cardiac tests at hospital ok, threw me out at 1 am in a blizzard.
Haven’t told them about CHS cause of a legal problem.
Still have the throbbing pain, just below sternum and slightly left of center (under rib as well).
Haven’t looked up Renal failure, any chance this is related?
Been two weeks without any weed in any form. Still feel crappy in morning, then ok midday, but early evening I start getting these chest pains.
Probably need to let a doctor in on the CHS and get a liver work up.
I would suggest that simply quitting might not be enough, there may some kind of damage that lingers (seems like everyones “leaps up” so quickly when they resume).
No liver issues, thank god.
Doc says quitting 30 years of daily pot use cold turkey is MAJOR stress to body.
R/X is rest, relax, destress and HYDRATE.
Swore out complaint against hospital for missing this a dozen times, despite me being very open and honest about my use and frequently mentioning showers. Doctor and Hospital education (espectially ER) is clearly indicated.
Keep you posted!
I’m a 62 year old woman who has smoked off and on for about 45 years. I may have missed about 4-5 years worth in that time trying to procure until Colorado passed it’s medical marijauna law. since then, I’ve been smoking every day except for vacations and sometimes then because we always vacation at home.
I have asthma and have found smoking the herb caused more coughing than necessary so I decided to try the concentrate which is provided through O-Pen and many others. It’s much cleaner, easier to deal with and it didn’t make me cough. However because of the nature of the product, I found myself needing more and more as the last year has played out. So I”m not blaming the concentrate but maybe the delivery method? Not sure if what suspends the concentrate caused what I have or not but I sure have been sick a lot this last year since consuming it. I still smoked the herb but at a much less amount that I had before because I had the concentrate to use. There’s been minimal talk about the concentrate so it may have nothing to do with it except that I smoked way too much using the concentrate.
So with that being said, around the holidays of 2015, I started getting sick. At first we thought it was altitude sickness because I was at 8200 feet compared to 5280 in Denver. I got sick then in Denver. Ok so it’s not altitude sickness. I play a lot of video games. Maybe the movement of the games could cause this. Still got sick when not playing the games. Ok so it’s not the games. then I thought maybe it’s nerves. I usually got sick when we went on vacation. I know right?! but I still got sick at home. At 1 point last year, I threw up 17 times in 1 day. Was taken to the ER. Got pumped up with 2 IVs and 2 throwup pills and still threw up on the way home. My doctor ran all kinds of blood work, stomach work, and found nothing wrong. HMMM why am I getting sick???
Finally the news had a story last Wednesday about CHS. I slapped my head and said finally someone has an answer. WAHOO. Now what do I do? So in reading everything I have, it would appear that it has grown toxic to me. I haven’t smoked it 6 days. Finally stopped throwing up. Still a little tentative with what I eat but am eating. Through all of this I have lost about 15 pounds between the 17 times in 1 day and this last bout. I had had about 6 of these occurrances in the last year. Not the best way to diet. I also understand that this might be causing my “elimination” problem over the last year as well. I’ve had diarhea off and off for about the same time.
The showers do help. I am exercising now that I”m eating better and picked up the fiber to help dispell the toxins.
Now comes the how to deal with loosing a very close friend. I quit smoking cigarettes 25 years ago and suppose that is what I will have to do here as well. It would appear that even with sesation, the problem could still be there. Go figure. It’s all good for those that like to drink to have that option but I don’t drink. So now I have to sit here sober while my whole family has a good time drinking and still smoking. Really sucks. I know I’m taking it out on the people I love and I hate that. I am at a loss for how to deal with this and feel very frustrated.
It’s good to know that there are other people out there suffering as I am. We are not alone in this even though the doctors might not care. I care about all of you and how you are doing with this and hope you are all getting better. But now what?
Just an update:
I did try to smoke after a two week break. Immediate problems with phlegm, up all night, miserable.
My original medical problems that I used cannabis for in the first place have spiked upward since I took the break.
Out of desperation, last night I tried some of my homemade edible oil. I boosted it with black pepper, a suggestion from another site.
I did have a very pleasant, very intense high, a great sleep, woke up w a little nausea but by no means unbearable. I “felt” like its not something I can do often, but it was a grand release and a welcome respite from events of the last month.
Recipees for oil abound and there is nothing particularly spectacular about my method, but if you want here are the particulars.
1) A little less weed than the recipee says, but good stuff (but very dried). Mine was organic and homegrown. I did do the fussy decarb (sp?) step this time.
2) mash the weed into preheated oil, especially if you use crock pot on warm method as I do.
3) use olive oil from CALIFORNIA not italy. Almost no oil from Italy is real, mostly from spain and never really virgin (like life)
4) add a couple of spoonfuls of an emulsifier.
5) Hour tops on “warm”
6) Strain and bottle in opaque booze bottles (I used Myers Rum) also gives you a poor spout.
7) One tablespoon max is strength I shoot for, I grind a little fresh back pepper directly into the spoon before I take it cold.
Thats it, don’t recommend rushing out and trying this if you haven’t done at least two week detox first, and even then be prepared for a CHS attack.
I got zero post nasal drip, excessive swallowing etc.
I have been a heavy marijuanna user since I was about 17. We’re talking smoking as soon as my feet hit the floor in the morning and smoking again as soon as I felt I was coming down from my high, all day every day. At 24 now, I have been going through this the last 3 years. The only time I haven’t got sick was when I wasn’t smoking. It took $6k+ in medical bills and multiple ER visits for me to find out from an ER NURSE, not doctor, that there was a condition called CHS. She asked me to talk to the physician that would be seeing me and asked me to be honest about my usage. I was. And lo and behold, first thing she asked when I said I smoked a lot of pot was if I was taking showers a lot. That was an understatement. I LIVE in the bathroom when these episodes hit. Scalding hot water and double doses of dissolvable zofran pills and phenergan suppositories are the only things that makes me feel better. I throw up anywhere from 1 to 20+ times a day, retching and dry heaving even after my stomach has been empty for days. My episodes usually last 2 weeks, and in that time I lose anywhere from 10 to 25 pounds. The last week has been another episode, however it hasn’t been as bad as previous episodes. I haven’t thrown up in almost 12 hours, but food is still yucky. Ice pellets have been my best friend. I have went through 50 pounds of ice in this one week alone. The only thing that has actually had a full bladder when I woke up this morning and it was such a relief to just pee. The racing heartbeat, headaches, adombinal pain, severe cold chills, random sweats, dizziness, lethargy, extreme nausea and vomiting and damage to my body wasn’t enough for me to quit smoking pot, so I am just having to distance myself from it now. It is such a relief knowing that I am not the only person that suffers from this condition. It breaks my heart that my favorite thing in the world making me sick. However it is comforting knowing I am not alone. More research desperately needs to be done with this to get to the root cause. I have literally wasted atleast 7 months of the last 3 years in a shower because of this mess. I have lost jobs, got into fights with my parents and boyfriend, almost wrecked while driving because I was so sick, and it just isn’t worth anymore. I know I’m going to have a rough time cutting it out completely. The longest I have went on my own without smoking was two months, and it was amazing how much better I felt. Just have to get in the right mind set and find support. Luckily I have had an awesome boyfriend the last 3 years that hasn’t left my side, except for work and to clean things up when this has happened. I have not smoked since January 9th, and am still having bouts of vomiting. But I know the end is near and I’ve made it this far. If anyone would like to discuss their experiences with this condition, or have found other ways of recovering from this faster, feel free to message me on facebook messenger. I have a black and white profile picture. Good luck to all of ya’ll going through this mess
I think I messaged you. Check your other folder?
I suffer from these symptoms. Not long ago I came across a grower who believes this is caused by an organic pesticide Neem oil and its active ingredient azadirachtin. I have been reading up on this pesticide and there is a strong case to be made this could be the problem.
The symptoms are the same and Neem grows in Au where we first started seeing this. Early 2000 neem became an commercial product in Australia.
Why do we not see this in some countries. And why do we see this where there is a culture of indoor grows?
I have been researching what could be causing my husband these terrible episodes for over 15 years. About 7 years ago, I happened on an article about CHS. I finally had an answer. I talked to my husband about it, and he scoffed it off. He was so sick for so many years. He had been to the ER many times. Went to the Dr and had liver enzyme testing done. Nobody had any answers. When we would run out of weed for a week or two, he wouldn’t get sick. He finally started coming around to the notion that MJ is what was making him sick. Then, last year, I got sick. Same symptoms, same exact problem. So we are both dealing with it. We are trying something new now. Smoke for a week, then stop for a week. If that works we may try 2 weeks of each, or 2 weeks of smoking and 1 week of abstinence. Trying to find a formula that works for us because of the many benefits of MJ for us both. My husband has RA and I have had depression and anxiety my whole life. MJ helps more than anything else does. So sorry for all that have to suffer with this. Don’t be stubborn about it. We all love it, but if your body rebels, it’s time to make some changes.
I started smoking pot and drinking at 15. By the age of 22 I was smoking and drinking like there was no tomorrow until I got the nausea, abdominal pain feeling. My first trips to the ER were the same as most they did all kinds of tests etc and nothing. I kicked drinking but continued to smoke. Fastforward to 2017 and I’m still with these symptoms. Yesterday I was ILL again with the same symptoms and the DR told me about CHS. I am not taking this serious as I was told about this in 2012 but didn’t listen to the doctor. After reading all these posts I feel that if you are going to be a heavy smoker you have to exercise to get those toxins out of your system. Use marijuana recreationally and don’t abuse it as most of us have. When I did exercise and drink and smoke I never had these symptoms jtd when I stopped exercising. I will start this time before smoking again a good work out routine and run. I know plenty of OGs that are 50+ years old smoking since 15 without these symptoms maybe because there work is more body demanding. Just my food for thought. Yes CHS is real but I have a strong feeling that exercising is the key and smoking moderately to where your body gives it time to get rid of the toxins it already has.
I am extremely active, and consider myself to be in good shape. I still had synptoms. Granted I was still smoking most hours of the day. I agree though, with moderation it would probably be fine. But even without the symptoms, I’m wondering if it’s damaging me perminantly in some way.
Does anyone know if I can still ingest it without having to worry about symptoms?
I am also wondering the same thing!! Can one take CBD capsules or oil? I suffer from inflammation (arthritis) and anxiety, and have heard it helps, but will it cause the same sickness after time also???
Probably not. I’m considering trying the same thing. I’ve done some research on CBD and I believe it will be the key to helping people with chronic CHS. It uses different receptors then THC and could be used to treat pot addiction and other pot related problems. I haven’t starting taking it yet but plan to very soon…
I have used marijuana for many years, but only two to three times a week, 3-5 tokes per usage. I have never experienced nausea, nor have I needed a hot shower for relief. My one and only problem, which has heretofore been undiagnosable (after several colonoscopys, a barium enema, several ct scans, and even a partial colectomy which did not relieve the symtom) is a type of pain in my lower abdomen, which is usually worst in the morning, but can last all day. It is not muscular, but it can inhibit range of motion. My question is simply this: how long after ceasing use will that symptom go away, assuming it is in some way cannabinoid induced? Thank you for your time
I’m 36 years old, female. I was very heavy pot smoker since the age of 15. For 10 years I suffered with this. It was hell, it brings me to tears thinking of what I went through. My only relief during these violently ill episodes were hot hot baths. After 2-3 days of the episode, I had to go to the ER for dehydration and pain medication, morphene, dilaudid, anything to knock me out and cease the pain and vomiting. No one knew what was wrong with me. Doctors started thinking I was an addict seeking pain medication, my family and friends hated seeing me go through these episodes. It was a horrendous, painful and an embarrassing period of my life. I wish the diagnosis was known back then. I was treated for severe anxiety and was told that the episodes were do to anxiety attacks. This made no sense to me, yes the episode made me very anxious because of the pain and uncontrollable vomiting but outside of the episodes I did not have anxiety. I quit smoking weed when I turned 30….I haven’t had an episode since! I had to self diagnose and the relief I have from now reading these articles is comforting. I never thought I would quit….I love smoking weed! I miss it, but I don’t miss ambulance rides to the hospital and the immense physical and psychological pain that came along with it. For those who are suffering, it does stop when you quit.
Well count me in. I’ve got 3yrs in this. No clue till I finally searched the hot bath+abdominal pain thing a month ago. Been puffing for 30yrs. ER, tests, doctors, med’s, and many dollars. Guess I took my last a week ago. Pesticides or pot, just to debilitating to take the chance again. So long good friend, hate to see you go. Thanks to this site and all the post’s. I think I’m the only one around here who has this. I don’t feel so alone anymore.
You’re not alone Jeffrey. I’ve been smoking continuously for about 35-40 years and have developed these symptoms about 20 years ago. I average about 7-10 ER visits a year. I go to a neurologist who actually prescribes Demerol. It helps more then other meds because it was invented as a anti-spasmodic and that’s exactly what it feels like is happening; complete intestinal spasms to the point they are “locked up” and nothing goes out the correct end! Today is the first day I’ve decided to try quitting pot. It’s been about 6 hours and I’m dying for a hit. I won’t take one though because I want to see if stopping will help. Unfortunately, so far it has… I’m afraid it will be the only way until more research is done. I have high (no pun intended!) hope for CBD. Good luck and know that those hours that you’re in the shower…there is somebody else trying to figure out why they are suffering.